Side effects to treatment
Treatment for kidney cancer include surgery, anti-cancer medication and radiotherapy. You might have side effects from any of these treatments. This page gives you advice on how to manage your treatment experiences to improve your quality of life.
Surgery

All surgery has some risks and complications. Possible complications of surgery to remove your kidney or part of your kidney (nephrectomy) include:
- Infection (your surgery wound becomes painful, red or swollen, leaks fluid or has an unpleasant smell).
- Bleeding (haemorrhage).
- Post-operative pneumonia.
- Rare allergic reactions to anaesthesia.
- A small risk of kidney failure if your remaining kidney is not working properly or you have kidney disease.
- Post-operative flank hernia.
If you have any of these complications, your healthcare team will manage them to make sure you recover fully from your surgery. For example, it is important that you keep your wound dry to avoid infection. If your wound becomes infected, you need to tell you healthcare team immediately. They will clean it and dress it and give you some antibiotics.
It is not unusual for cancer patients to become constipated because of pain medications and lack of exercise after surgery. Changing your diet to a high fibre diet and increasing your intake of water can help relieve constipation. If this is not successful, you might need to take laxatives.
Excessive bleeding (haemorrhage) might occur immediately after surgery. Your surgeon will stop the bleeding and, depending on the amount of bleeding, you might need to have a blood transfusion.
Some patients develop a bulge (hernia) at the site of their wound. A hernia is a gap in the muscle wall of the abdomen that allows the internal organs to push out. Hernias are sometimes monitored and do not always need repairing. However, some hernias can cause serious problems. The only way to repair a hernia is to have more surgery. Your healthcare team will be able to give you advice about the management of a hernia.
Anti-cancer medication
 When you are given medication for your kidney cancer, you might have some side effects. The side effects to some medications are well known and can be managed by you and your healthcare team, especially your cancer nurse. The sooner side effects are reported to your healthcare team, the easier they are to treat and manage so they do not affect your life. You should be made aware of the common side effects to kidney cancer treatments so that you can start to manage them at home. Effective management of side effects improves tolerance to treatments and increases the benefits of treatment.
When you are given medication for your kidney cancer, you might have some side effects. The side effects to some medications are well known and can be managed by you and your healthcare team, especially your cancer nurse. The sooner side effects are reported to your healthcare team, the easier they are to treat and manage so they do not affect your life. You should be made aware of the common side effects to kidney cancer treatments so that you can start to manage them at home. Effective management of side effects improves tolerance to treatments and increases the benefits of treatment.
Common side effects and how they are managed include the following:
High blood pressure
Understand what is normal for you, monitor for high blood pressure, record your blood pressure daily, stop smoking, reduce the amount of caffeine, salt, saturated fats and sugar in your diet, exercise regularly, see your hospital team or GP to treat high blood pressure with anti-hypertensive medication, if needed.
Diarrhoea
If you have diarrhoea, it is important to let your healthcare team know as soon as possible. You need to understand your bowel movement habits, change your diet (small, regular meals, drink plenty of water, use probiotics, increase consumption of bananas, rice, chocolate, bread, reduce consumption of high fibre food, beans, and seeds), see your hospital team or GP to prescribe diarrhoea medication, if needed.
Skin rashes
Check your skin daily, use emollient-based creams for a mild to moderate rash, e.g., zinc oxide or lanolin-based emollients, oatmeal lotion or steroid cream, wear protective clothing, use oral prednisolone for moderate to severe rash, see your hospital team or GP to or a dermatologist if the rash continues. Steroid cream or prednisolone should only be taken if prescribed by your healthcare team.
Sore mouth (stomatitis)
Keep your teeth and mouth clean, make sure you don’t irritate your mouth, avoid spicey food, acidic food, like lemons, crunchy food, smoking, and alcohol, eat soft food cut into small pieces, use straws to drink through, avoid oral rinses with alcohol. See your hospital team or GP to prescribe medications or nutritional support if eating or loss of appetite becomes a problem.
Extreme tiredness (fatigue)
Understand the cause of your fatigue and rule out any other conditions that may be causing fatigue, pace your activities to save your energy, organise your home and work in a way to help you cope with less energy, take regular, gentle exercise and a healthy diet, relaxing activities, such as reading, listening to music, watching TV, and a short sleep during the day, relaxation techniques, such as meditation, yoga, and massage, have a regular sleep pattern, eat and drink well.
Reduced appetite/weight loss
Try to eat nutritious, high-calorie, high protein foods, like eggs, fish, cheese, and meat, don’t eat food that causes you to have diarrhoea, keep your teeth and mouth clean, avoid fad diets, see your hospital team or GP to or a dietitian if you continue to lose weight or can’t eat.
Nausea and vomiting
Eat small meals regularly each day, drink plenty of water, eat bland, easy to digest food, such on sugar-free mints or sweets, keep your teeth and mouth clean, avoid too hot or too cold food and drink, chocolate, caffeine, alcohol, smoking, and strong smells, try relaxation therapies. See your hospital team or GP to treat with medication to treat nausea and vomiting, if needed.
Sore hands and feet (palmar plantar erythrodysaesthesia, PPE)
Observe good nail hygiene and have regular manicures and/or pedicures. Use moisturising creams and exfoliating creams. Wear cotton gloves and socks. Protect your hands and feet, especially the pressure-sensitive areas. Avoid contact with hot water, trauma, friction and excessive pressure. Wear a high sun-protection factor (factor 30 or above).
Immunotherapy side-effects
Immunotherapy can cause immune-related side effects. Most immune-related side effects are not long-lasting and will settle in time. They can affect many parts of the body. The most common ones are: skin rash, gut problem like colitis, fatigue, and joint pain. The only long-lasting side effects are those affecting the glands: thyroid (hypothyroidism), pancreas (diabetes), adrenal (adrenal insufficiency), and pituitary (hypophysitis). These side effects may be worse if you are taking combinations of immunotherapies for advanced kidney cancer. Most immune-related side effects can be managed either with simple monitoring or with medication that suppresses the immune system (immunosuppressants), especially if found and treated early.
Radiotherapy
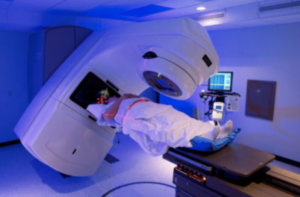 A special form of radiotherapy called stereotactic radiotherapy is sometimes used to treat kidney cancer. Stereotactic radiotherapy uses a high dose of radiation targeted at the tumour. This aims to kill all the cancer cells in that area.
A special form of radiotherapy called stereotactic radiotherapy is sometimes used to treat kidney cancer. Stereotactic radiotherapy uses a high dose of radiation targeted at the tumour. This aims to kill all the cancer cells in that area.
Radiation can cause side effects during or immediately after treatment. They tend to disappear gradually after radiation is complete. Possible immediate side effects depend on the area being treated. They include:
- Extreme tiredness (fatigue).
- Reddening, irritation and swelling of the tissues in the treatment area.
- Loss of body hair in the treatment area.
- Feeling or being sick (nausea and vomiting).
Stereotactic radiotherapy is very precise and targets the tumour with limited damage to healthy surrounding tissue. This minimises the possible side effects of the treatment.
Tell you healthcare team about any side effects to treatment as soon as possible. The earlier they are reported, the easier they are to treat and manage. For some side effects, you might need to see a specialist doctor or nurse to help you manage them, such as an endocrinologist, palliative care doctor or nurse, a dietitian, or a physiotherapist.
If you have other conditions, such as heart disease or lung disease, you might need to see a doctor specialising in these conditions to support you during your cancer journey. Some cancer treatments might make other health conditions worse, like high blood pressure, so it is important that you see a specialist doctor to help you manage these side effects.
Patient guides
The following patient guides from the European Society for Medical Oncology (ESMO) have been prepared to help you, as well as your family and carers, better understand and manage immunotherapy-related side effects and cancer pain. The immunotherapy patient guide contains information on the most common side effects to immunotherapies, how your healthcare team will manage these symptoms, and a few strategies you can use yourself to minimise their effects. The cancer pain patient guide has been prepared to help you better understand cancer pain and its treatment. It contains up-to-date guidance on the types of treatments that may be available and any possible side effects of treatment.
You can also learn how other patients have managed some of the common side effects to anti-cancer medication for advanced kidney cancer from our help sheets, which can be found by clicking here.


