Share this Page:
A recent study, published in the journal Cancer Discovery, has identified how kidney cancers spread (metastasise) to other parts of the body by hijacking genes from other cell types and taking on their functions.
The study was led by scientists from the Medical Research Council (MRC) Cancer Unit at the University of Cambridge. The researchers suggest that the findings from the study may also help to explain how other types of cancers spread and may help in the development of new treatments for cancer.
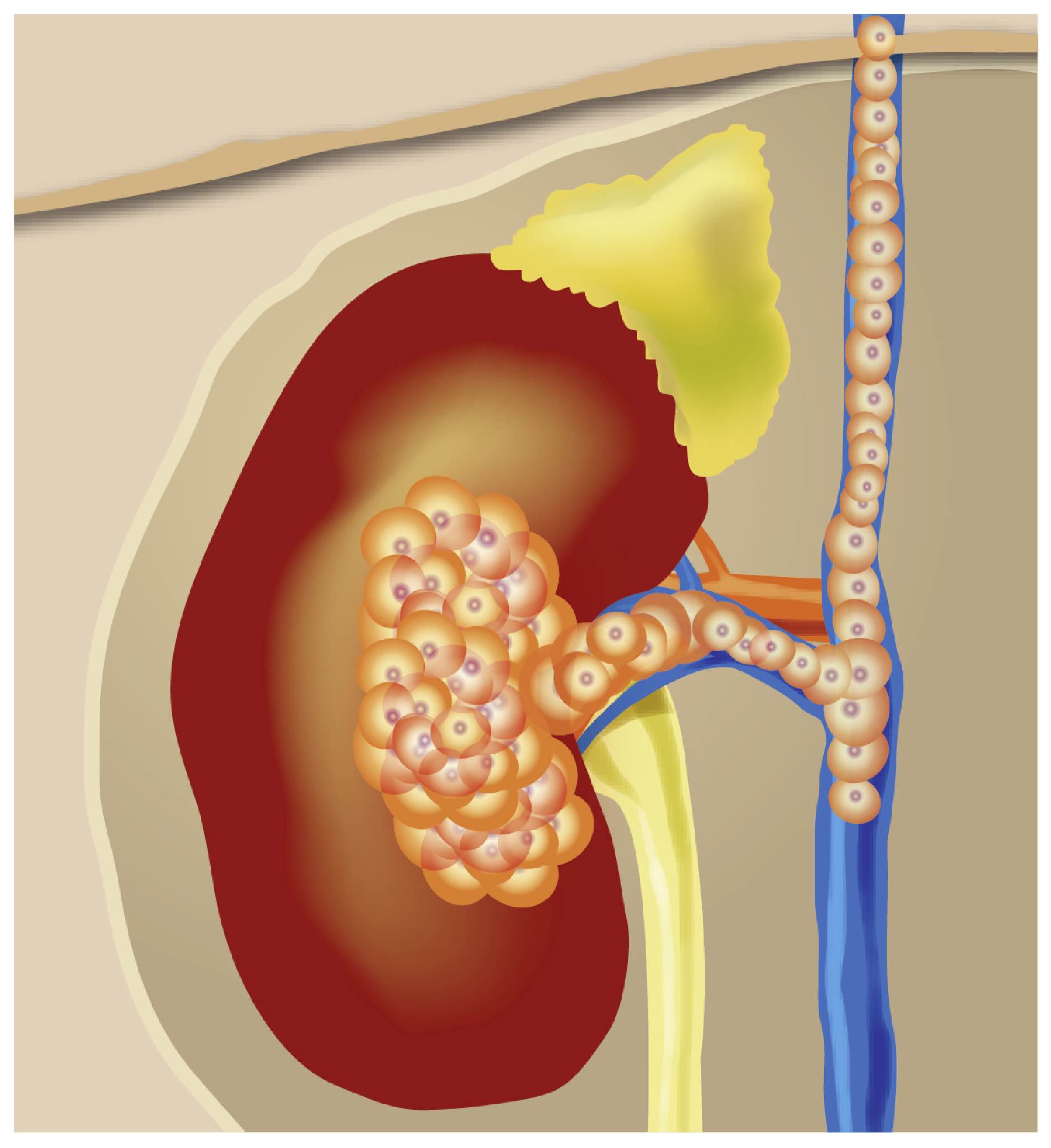
When cancer cells metastasise, they need to be able to break away from the original tumour, survive in the blood stream, and invade another organ to form a secondary tumour (metastasis).
Using experimental models with cancer cells from mice, the scientists found that genes that are normally turned off in kidney cells were turned on in the cancer cells – the cancer cells had hijacked genes that are normally turned on in white blood cells (cells that are part of the immune system and fight diseases) to help the cancer metastasise.
The scientists compared their findings in the mouse model to kidney cancer samples from hundreds of people with clear cell renal cell carcinoma (RCC). Similar genes were activated in the human RCC cells, which suggests that what they saw in the mouse model may be happening in human cancers.
Dr Sakari Vanharanta from the MRC Cancer Unit at the University of Cambridge and senior author on the paper, said: “How cancers develop the capability to spread is a long-standing problem that hasn’t been fully answered by searching for mutations in genes. We show for the first time how cancers can steal the activity of specific enhancers – genetic regions which turn genes on and off – to activate genes from different tissue types. Activating these genes allows the cancer cells to steal features from normal cells, which facilitates their spread in the body.
“Metastasis is responsible for the majority of cancer-related deaths and this discovery helps us better understand how cancers spread and could provide new targets for cancer drugs that limit the capability of cancer cells to activate genes that should be switched off.”
The researchers still do not understand what causes these changes in gene activation in the cancer cells.
Dr Nathan Richardson, Head of Molecular and Cellular Medicine at the MRC, said: “Understanding what enables cancers to metastasise and establish secondary cancers around the body is hugely important in our quest to tackle this disease and reveal new approaches to treatment.”